Final AHC Reporting
Background
Health Net of West Michigan was one of 28 organizations across the United States selected to participate in the Accountable Health Communities Model (AHC), a national initiative led by the Centers for Medicare & Medicaid Services from 2017 to 2022.
The AHC Model focused on identifying and addressing health-related social needs, also known as social determinants of health, through screening and navigation services. These efforts aimed to better understand and respond to non-medical factors that influence health outcomes.
Throughout the project, screening efforts focused on five key areas:
- Housing instability
- Utility needs
- Food insecurity
- Transportation
- Interpersonal safety
Evaluation Efforts
At the beginning of the AHC project, a central hypothesis guided the work:
- Beneficiaries who received navigation services would have greater resolution of their social needs than those who did not receive navigation services. This would lead to better health outcomes and reduced health care expenditures.
However, the findings from the national evaluation (2020 to 2026) revealed a more complex story:
- Finding: Beneficiaries who received navigation services had similar rates of need resolution compared to those who did not.
- At the same time, there were consistent reductions in hospital-based utilization and overall healthcare expenditures among those who received navigation support.
- Conclusion: The impact of the AHC Model extends beyond simple need resolution, suggesting that its benefits are driven by more nuanced mechanisms, with evaluators concluding “navigation itself may be a key mechanism of change.”
Understanding AHC’s Impact
As researchers examined the results more closely, several key factors emerged that helped explain these outcomes:
- Trusted relationships matter: Building strong, consistent relationships with resource navigators may increase trust not only in the navigator but also in the healthcare system as a whole.
- Navigators go beyond referrals: Interviews revealed navigators often provided support well beyond connecting clients to resources, like reminding individuals about critical medical or mental health appointments.
- Relational care drives engagement. The trust developed between navigators and community members likely enhanced the effectiveness of navigation services even when needs were not fully resolved.
- Some populations benefit more. Certain groups, particularly individuals with chronic conditions, were more likely to experience both need resolution and reductions in healthcare utilization and costs.
- Partial solutions still matter. Even addressing part of a need can improve outcomes. For example, helping someone access transportation for medical appointments, even if other transportation challenges remain, can lead to better health outcomes.
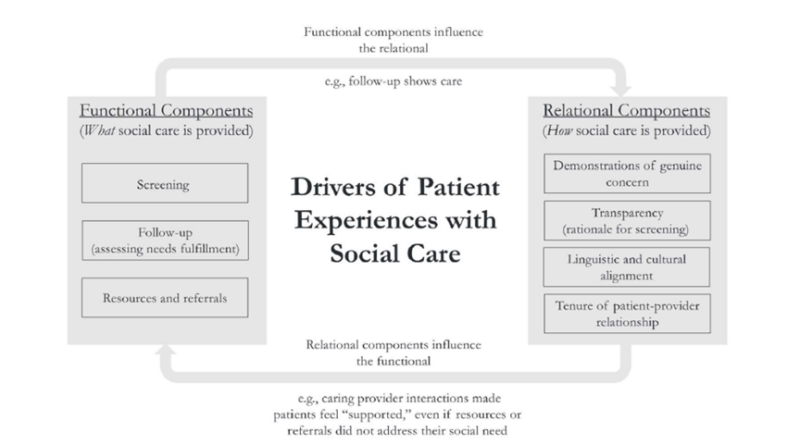
These findings are reinforced by emerging research showing that the experience of being supported and heard plays a critical role in healthcare-based social care, regardless of whether a need is fully resolved.
Impact on Our Community
The AHC Model has had a lasting influence on how Health Net of West Michigan and our partners approach community care. Since the conclusion of the project, these efforts have not only continued but also grown and evolved.
- Our Care Model © was heavily influenced by AHC learnings; it emphasizes relationship-building, cultural humility, and empowering individuals to achieve their goals.
- Expanding training and collaboration. To date, 37 organizations have participated in Care Model Training © strengthening the skills and confidence of resource navigators while fostering a more connected network of providers.
- Standardized social needs screening. Screening for health-related social needs is now increasingly embedded as a standard of practice in healthcare settings, helping identify needs earlier and more consistently.
- Demonstrating real impact. The AHC Model reinforces what we see every day: resource navigation improves health and well-being while helping reduce healthcare costs.
Resources and References
- Potharaju, K., Gottlieb, L. M., Wing, H. E., Gonzalez‐Rocha, A., Brewster, A. L., Jones, D. H., & Quiñones‐Rivera, A. (2025). Drivers of Patient Experiences With Healthcare‐Based Social Care. Health Services Research, 61(1), 1–9. https://doi.org/10.1111/1475-6773.70020
- Bryant A, Walsh-Felz A, Jacklitz J, Lindberg S. The Impact of a Community Resource Navigator Program on Patient Trust. WMJ. 2020 Sep;119(3):190-193. PMID: 33091287; PMCID: PMC9125772. https://pmc.ncbi.nlm.nih.gov/articles/PMC9125772/
- Teggart K, Neil-Sztramko SE, Nadarajah A, Wang A, Moore C, Carter N, Adams J, Jain K, Petrie P, Alshaikhahmed A, Yugendranag S, Ganann R. Effectiveness of system navigation programs linking primary care with community-based health and social services: a systematic review. BMC Health Serv Res. 2023 May 8;23(1):450. doi: 10.1186/s12913-023-09424-5. PMID: 37158878; PMCID: PMC10165767. https://pmc.ncbi.nlm.nih.gov/articles/PMC10165767/#Sec24
- Renaud, J., McClellan, S.R., DePriest, K., et al.: Addressing Health-Related Social Needs Via Community Resources: Lessons From Accountable Health Communities. Health Affairs. 42(6):832-40, 2023. https://doi.org/10.1377/hlthaff.2022.01507
- https://www.cms.gov/priorities/innovation/innovation-models/ahcm



